
Retrograde pyelogram – Any pyelogram in which contrast medium is introduced from the lower urinary tract and flows toward the kidney (i.e. In a 'retrograde' direction, against the normal flow of urine). Anterograde pyelogram (also antegrade pyelogram) – Any pyelogram where a contrast medium passes from the kidneys toward the bladder. The primary use of retrograde pyelography is to evaluate suspected ureteral obstruction or ureteral urothelial cancer in a patient whose ability to excrete contrast.
Retrograde Pyelogram What is a retrograde pyelogram?A retrograde pyelogram is an imaging test that uses X-rays to look at your bladder,ureters, and kidneys. The ureters are the long tubes that connect your kidneys toyour bladder. This test is usually done during a test called cystoscopy. It uses anendoscope, which is a long, flexible, lighted tube.
During a cystoscopy, the healthcareprovider can inject contrast dye directly into the ureters. The contrast helps partsof the body show up more clearly on an X-ray. The exam is done using anesthesia.Why might I need a retrograde pyelogram?You may need a retrograde pyelogram if your healthcare provider thinks something isblocking your kidneys or ureters. It is also used to find a possible causes of bloodin your urine. This may be a tumor, stone, blood clot, or narrowing (strictures).The test is also used to check the placement of a catheter or a ureteral stent. Astent is a hollow tube that lets urine pass around a blockage.This test can typically be done even if you are allergic to contrast dye. Only a smallamount of the dye is absorbed by the body.
The test may also be done if you have poorkidney function.Your healthcare provider may have other reasons to recommend a retrograde pyelogram. What are the risks of a retrograde pyelogram?You may want to ask your healthcare provider about the amount of radiation used duringthe test. Also ask about the risks as they apply to you.Consider writing down all X-rays you get, including past scans and X-rays for otherhealth reasons. Show this list to your provider. The risks of radiation exposure maybe tied to the number of X-rays you have and the X-ray treatments you have over time.Tell your healthcare provider if you:.Are pregnant or think you may be.
Radiation exposure during pregnancy may lead tobirth defects.Are allergic to or sensitive to any medicines, contrast dye, or iodine. Because contrastdye is used, there is a risk for allergic reaction to the dye.Have kidney failure or other kidney problems. In some cases, the contrast dye cancause kidney failure. You are at higher risk for this if you take certain diabetesmedicines.Possible complications of retrograde pyelogram include:.Sepsis.Urinary tract infection.Bladder tear.Bleeding.Nausea or vomitingYou may not be able to have this test if you are severely dehydrated.You may have other risks depending on your specific health condition. Talk with yourprovider about any concerns you have before the procedure.Certain things can make a retrograde pyelogram less accurate.
These include:.Stool or gas in your intestines.Barium in your intestines from a past barium testHow do I get ready for a retrograde pyelogram?.Your healthcare provider will explain the procedure to you. Ask him or her any questionsyou have about the procedure.You may be asked to sign a consent form that gives permission to do the procedure.Read the form carefully and ask questions if anything is not clear.You'll need to fast for a certain time before the procedure. Your healthcare providerwill tell you how long to fast, whether for a few hours or overnight.Tell your healthcare provider if you hare pregnant or think you may be.Tell your healthcare provider if you've ever had a reaction to any contrast dye, orif you're allergic to iodine.Tell your healthcare provider if you're sensitive to or are allergic to any medicines,latex, tape, and anesthesia.Tell your healthcare provider of all prescription and over-the-counter medicines andherbal supplements that you're taking.Tell your healthcare provider if you have a history of bleeding disorders. Also tellyour provider if you're taking any anticoagulant (blood-thinning) medicines, aspirin,or other medicines that affect blood clotting. You may need to stop these medicinesbefore the test.You may need to take a laxative the night before the test and have a cleansing enemaor suppository a few hours before the test.You may get a sedative before the procedure to help you relax. Because the sedativemay make you drowsy, you'll need someone to drive you home.Follow any other instructions your provider gives you to get ready.What happens during a retrograde pyelogram?You may have a retrograde pyelogram as an outpatient or during a hospital stay.
Wymer, in, 2010 Retrograde PyelographyRetrograde pyelography is performed when the ureters are poorly visualized on other imaging studies or when samples of urine need to be obtained from the kidney for cytology or culture. Patients who have severe allergies to contrast agents or impaired renal function can be evaluated with retrograde pyelography. The examination is performed by placing a catheter through the ureteral orifice under cystoscopic guidance and advancing it into the renal pelvis. With use of fluoroscopy, the catheter is slowly withdrawn while radiographic contrast material is injected (see Figs. 58.4 and 58.13 Fig. This technique provides excellent visualization of the renal pelvis and ureter and can be used for cytologic sampling from suspect areas.
Kitt Shaffer, in, 2010 INTRAVENOUS AND RETROGRADE UROGRAPHYThe advent of CT and ultrasound has markedly decreased indications for IV and retrograde urography. In an IV pyelogram, after injection of a bolus of IV contrast material, radiographs and tomograms are obtained rapidly to demonstrate the enhancement of the renal parenchyma, followed by more delayed radiographs to show the contour of the collecting systems, ureters, and bladder. Filling of the collecting systems is highly variable, and it is not uncommon for small segments of the ureters to be poorly visualized.
If small mucosal lesions of the collecting system are suspected, retrograde studies may be preferable. Cystography involves filling the bladder with contrast via catheter, usually under fluoroscopic guidance. To visualize the urethra, the catheter can be withdrawn after filling of the bladder and radiographs obtained during urination in a voiding cystourethrogram (VCUG).
In conjunction with cystoscopy, the ureters can also be cannulated and retrograde injections may be performed into the collecting systems under fluoroscopic guidance. This provides the best visualization of the entire collecting system. The cost for an IV pyelogram is approximately 3.25 cost units, and the radiation dose is 3–6 cG. The cost of a cystogram is approximately 1.5 cost units, a VCUG is 2.25 cost units, and a retrograde CUG is 2.5–3 cost units. The radiation dose is 3–6 cG, with particularly high gonadal doses for the VCUG. This radiographic study is rarely necessary to diagnose UPJ obstruction.
In a series of 108 children undergoing pyeloplasty, retrograde pyelography (RPG) did not change the surgical approach or planned procedure in any of the cases. 61 However, RPG is still commonly performed before open pyeloplasty.
The reason for this is simple. During the diagnostic process, information regarding the exact anatomic location of the UPJ in relation to other anatomic structures is lacking. Therefore to precisely identify the location of obstruction and perhaps exclude the presence of another distal obstruction, RPG is performed ( Figs. 113-11 and 113-12). 1.Intravenous urography: A urogram may demonstrate partial obstruction, hydroureteronephrosis, and drainage into the vagina.
2.Cystoscopy and retrograde pyelography are performed to evaluate for bladder injury and to visualize the distal ureteral segment if not well seen on the urogram. An attempt at retrograde stenting is reasonable if the pyeloureterogram demonstrates ureteral continuity. Prolonged internal diversion with ureteral stenting may result in resolution of the fistula.
3.CT/MRI: Cross-sectional imaging may be useful to evaluate for pelvic malignancy when indicated or to evaluate for a urinoma in patients with persistent fevers. 4.Cystogram or cystometrogram: In cases in which a long segment of distal ureter is involved and a Boari flap is being considered for reconstruction, a cystogram or cystometrogram may be useful to evaluate the bladder capacity. In addition, a cystogram should evaluate for vesicoureteral reflux. Paz, in, 2014 Pyelography.Radiopaque dyes are used to radiographically examine the urinary system. Two types of tests are performed: intravenous pyelography (IVP) and retrograde urography.Intravenous pyelography consists of (1) taking a baseline radiograph of the genitourinary system, (2) intravenous injection of contrast dye, and (3) sequential radiographs to evaluate the size, shape, and location of urinary tract structures and to evaluate renal excretory function.
The location of urinary obstruction or cause of nontraumatic hematuria may be also be identified with this procedure. 6,9,11Retrograde urography consists of passing a catheter or cystoscope into the bladder and then proximally into the ureters before injecting the contrast dye. This procedure is usually performed in conjunction with a cystoscopic examination and is indicated when urinary obstruction or trauma to the genitourinary system is suspected. Evaluation of urethral stent or catheter placement can also be performed with this procedure. Wymer, David T. Wymer, in, 2019 4.
What is retrograde pyelography?The injection of contrast material directly into the distal ureter or the ureteral orifice of the bladder for visualization of the collecting system and ureter, without relying on the ability of the kidneys to excrete contrast media. The primary use of retrograde pyelography is to evaluate suspected ureteral obstruction or ureteral urothelial cancer in a patient whose ability to excrete contrast material is significantly impaired.This is an adjunctive technique when conventional imaging studies fail to adequately demonstrate the suspected pathology. Retrograde pyelography does not evaluate the kidney parenchyma and requires cystoscopy to place the catheters. This procedure is usually performed by a urologist.An alternative to the retrograde pyelography is antegrade pyelography, usually performed by an interventional radiologist.
A percutaneous needle is placed into the kidney collecting system, and contrast is injected. 1.Preliminary cystoscopy is required. 2.A ureteral orifice is identified and catheterized with a catheter, usually 5 F. The catheter is advanced to the renal pelvis and contrast is instilled. The same contrast agents employed for IVU or CT are used for retrograde pyelography. To opacify the ureter alone, the ureteral orifice is occluded with a bulb occlusion catheter and contrast injected while a film is obtained. 3.Films—a preliminary KUB film is essential.
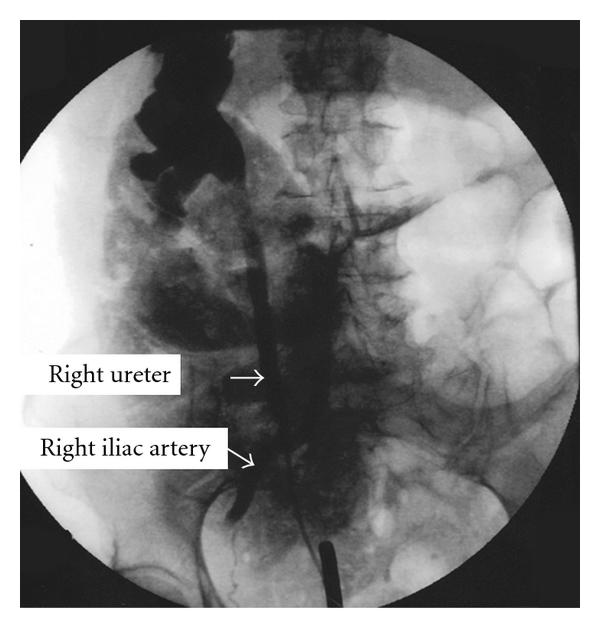
After contrast injection, films are obtained to delineate unopacified or poorly seen portions of the collecting system or ureter in question. If obstruction is suspected, a film is also obtained several minutes after removal of the ureteral catheter to evaluate the drainage of the collecting system. 4.The use of fluoroscopy is an important adjunct to RPG. In most hospital settings, however, this requires the placement of a ureteral catheter in the cystoscopy suite and the subsequent transport of the patient to the radiology department for catheter injection. 5.RPG may be impossible in some patients, such as those with very larger prostates, in whom the gland overlies the ureteral orifices, preventing proper catheter placement. At times, even though the orifice is identifiable, it may not be possible to catheterize it, such as may occur with tortuous ureters or after ureteral reimplantation.
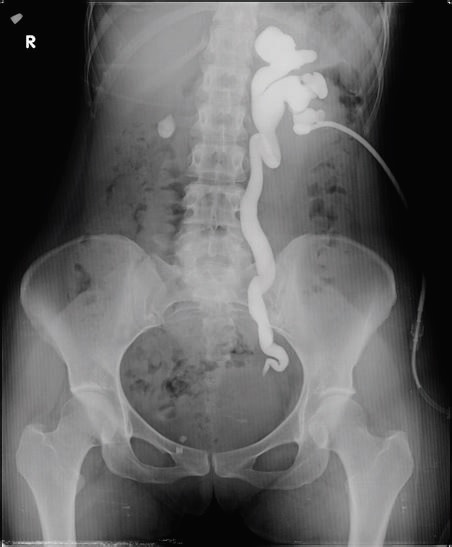
1.Radiologic studies. A)Intravenous excretory urography. Either a fixed radiolucent defect or nonvisualization of part or all of the collecting system is noted. Stippled calcifications may also be seen on the plain film. B)Retrograde pyelography is indicated to evaluate pyelocalyceal and ureteral segments not adequately visualized on excretory urography, given its greater sensitivity. Upper tract tumors demonstrate filling defects in up to 75% of cases.
C)CT may help to differentiate a renal parenchymal mass from a renal pelvic mass or a ureteral tumor from a radiolucent calculus. It may evaluate for the presence of hilar or periureteral lymphadenopathy. D)Although ultrasonography may delineate nonopaque calculi from a soft tissue density, its use is limited in tumor staging. 2.Brush biopsy/cytology. This is usually performed during pyeloureterography and may be done by a urologist or radiologist. Although the combination of an upper tract filling defect and a positive renal wash cytology in the same side is sufficient evidence for definitive surgical treatment, ureteroscopy may identify multifocal tumors.
However, a renal wash cytology positive for TCC without the presence of urothelial filling defects on urography mandates further evaluation with ureteroscopy. 3.Ureteroscopy allows direct visualization and biopsy of the upper tract urothelium.
In addition, laser photocoagulation of the lesion may be performed in patients with small, low-grade lesions, a solitary kidney, or in the setting of compromised renal function. Nephroscopy may also allow direct biopsy, resection, ablation, or fulguration of renal pelvic or ureteral tumors if retrograde access if not feasible.

